Acid reflux is the term used to indicate that stomach contents flow back into the esophagus. Acid reflux is common in both children and adults, and anti-reflux medications are among the most commonly prescribed. Usually symptoms are limited to a burning sensation, at the level of the stomach or higher, and sometimes a bitter taste at the back of the mouth. Depending on the amount and frequency with which acid reflux occurs, reflux causes real problems. For example, the acidic stomach contents can cause damage to the esophagus, larynx or lungs.
The first time I heard about voice problems due to acid reflux, I was very surprised by this. After all, the vocal folds do not normally come into direct contact with gastric juices. When I checked with colleagues, several were aware of the connection between acid reflux and voice problems; one colleague even had a student who had to stop her singing studies for this reason. Also, a family member was recently prescribed medication for acid reflux, even though she had asthmatic symptoms rather than stomach problems. So acid reflux can, sometimes without you knowing it, be the cause of serious complaints and also the cause of voice problems
Sphincter muscles
In the transitional area between the esophagus and stomach, there is a sphincter muscle (a circular muscle) called the lower esophageal sphincter. And also at the top of the esophagus, in the transition area from the esophagus to the throat, is a sphincter muscle called the upper esophageal sphincter. These sphincters allow what wants to go down (food and drink) to pass smoothly, but close when something wants to go up. They are not always closed. You need to be able to burp, and if you are nauseous, you need to be able to vomit. The sphincters are controlled by nerves. These cause the sphincters to relax when there is too much tension on the stomach. In this way, air, for example, can escape. When the stomach contents rise to the surface, it is called acid reflux. In itself, this is not a disease. Acid reflux disease only occurs when the sphincters are relaxed too often and for too long.
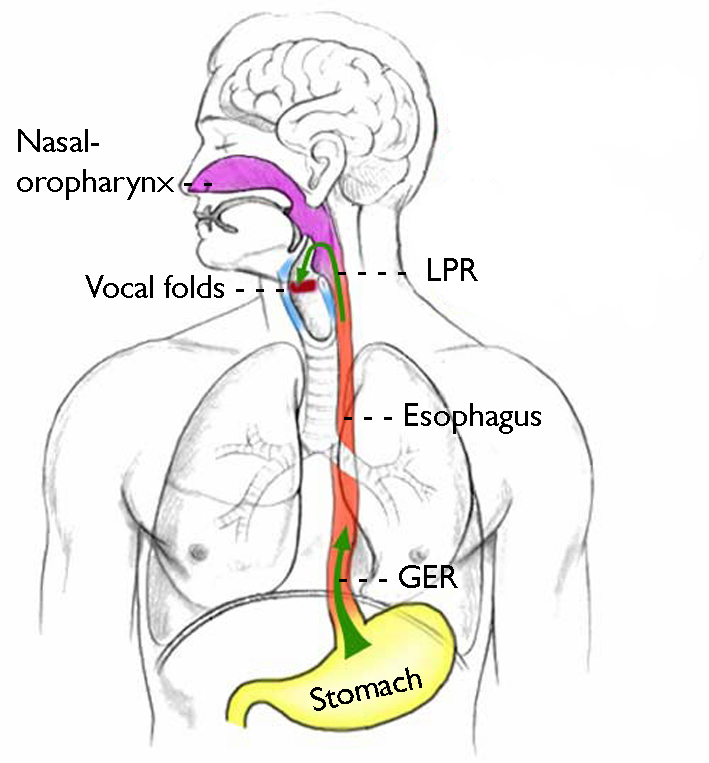
Two types of reflux
There are two types of acid reflux. When only gastric juice flows back into the esophagus and affects the mucous membranes there, it is called gastroesophageal reflux disease (GER or GERD). This form does not cause voice problems. When stomach acid also enters the throat, larynx and/or trachea, it is called laryngopharyngeal reflux disease (LPR or LPRD). The latter is damaging to the vocal folds, among other things, because the stomach acid irritates the mucous membranes of the vocal folds.
Voice problems
Studies by Belafski et al (2002) and Byrne et al (2006) show that LPR plays a role in 50% of voice problems. Due to the irritation of the vocal folds, LPR is associated with the development of granulomas (a certain type of swelling of the connective tissue), the development of vocal fold nodules, the development of cancer of the larynx, hoarseness and also with symptoms such as feeling a lump in the throat.
Hidden reflux
It is possible to suffer from acid reflux (especially in LPRD) without that acidic taste and burning sensation. In this “hidden reflux” or “silent reflux” the cause of the symptoms is more difficult to detect. The esophagus in this case may be inflamed, there may be problems such as hoarseness, asthma, excess mucus on the vocal folds, frequent throat scraping, difficulty swallowing, coughing, pneumonia and breathing problems. An extreme morning voice may also indicate that you are dealing with acid reflux. In this case, when you get up, your voice has a lot of trouble singing high notes, takes a long time to warm up, and the entire vocal range does not return until later in the day. Other symptoms may include waking up with a bitter taste in your mouth and a raspy, irritated feeling around the larynx and at the back of the throat. This form of acid reflux occurs at all ages.
The causes
Acid reflux can be caused by the malfunctioning of the lower and/or upper sphincter of the esophagus. There may also be problems with the peristaltic movement of the esophagus, which in a normal situation causes the contents of the esophagus to move toward the stomach. Smoking and obesity also increase the risk of acid reflux. Alcohol, caffeine, peppermint and chocolate negatively affect the function of both sphincters, increasing the risk of acid reflux symptoms.
The diagnosis
Because the symptoms are not very specific, it is difficult to diagnose LPRD. The relationship between the symptoms and the possible cause is not always seen. Speech therapists do use questionnaires to determine acid reflux. ENT physicians, in addition to naturally questioning their patients, may use various tests to diagnose reflux. The most commonly used are gastroscopy (looking into the stomach with an endoscope) and laryngoscopy. Sometimes a trial treatment with antacids is prescribed to see if it reduces the voice symptoms. To make a proper diagnosis of acid reflux, it is usually necessary to collect several pieces of information.
Treatment
A doctor will usually treat acid reflux symptoms with medication. These medications are designed to reduce stomach acid production or neutralize acidity in the stomach. At first, the medication may seem to make the symptoms worse, but it is actually important to keep the medication on long enough. Dr. Pahn (of the Nasal Method) also urges you to never stop the medication abruptly, but always taper it off slowly. It is also important to know that some antacids cause hoarseness because they have a drying effect on the mucous membranes of the larynx. These medications are therefore not recommended for LPR symptoms.
Sometimes a speech therapist is referred to because of the voice problems. A speech therapist cannot do anything about the cause of the symptoms, but can reduce the vocal load by learning a more efficient vocal technique. The same applies to the vocal pedagogue.
What can you do yourself?
There are also a number of actions you can take yourself to reduce acid reflux symptoms: When you lie down, for example in bed at night, heartburn rises more easily. Therefore, try to raise the headboard of your bed and do not lie down immediately after eating. For the same reason, it is best not to eat two to three hours before you go to bed. Avoid coffee, black tea, alcohol, carbonated drinks, chocolate, peppermint and hot spicy food. Do not eat too much and not too fat and prefer to eat several small portions rather than a small number of large ones. Reduce weight if you are overweight and stop smoking. Eat slowly and chew well and allow hot drinks and food to cool a bit first. Furthermore, tight clothing can put unwanted pressure on the stomach, and bending over also increases pressure on the stomach.
Published in the Bulletin of the Dutch Association of teachers of Singing. October 2010